top of page
Patient Presentation: A 23-year-old obese female was diagnosed with idiopathic intracranial hypertension (IIH) and referred to neurosurgery for ventriculoperitoneal shunt. A baseline ocular examination was performed prior to the procedure.
On examination, vision was 20/200 in the right eye, and 20/40 in the left eye. There was a right relative afferent pupillary defect. Slit lamp examination was normal.
A dilated fundus examination was performed demonstrating the following:
Retina
Case 43
Patient Presentation: A 28-year-old female with no past ocular history presented to emergency clinic with decreased vision OD. Her visual acuity was 20/25 OD and 20/20 OS. Colour vision was 14/14 on Ishihara plates OU. Fundus photos and OCT macula OD is shown below:


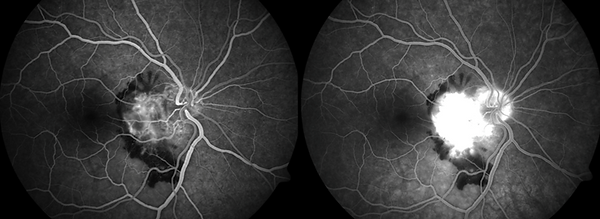
Question: An intravenous fluorescein angiography (IVFA) was conducted and demonstrated hyper-fluorescence that increases both in size and intensity in the late phase. What is the most likely diagnosis?
References:
1. Jutley G, Jutley G, Tah V, Lindfield D, Menon G. Treating peripapillary choroidal neovascular membranes: a review of the evidence. Eye (Lond) 2011;25(6):675-81.
2. SR Singh, AT Fung, S Fraser-Bell, et al. One-Year Outcomes of Anti-Vascular Endothelial Growth Factor Therapy in Peripapillary Choroidal Neovascularisation. Br J Ophthalmol 2019;EPub Ahead of Print.
bottom of page
.png)